Are psychedelics the new wonder drugs for mental health? Given the excitement surrounding the field, one could be forgiven for thinking so. The research is promising, patient interest is growing, and more practitioners are seeking training in psychedelic-assisted approaches. But it is also a young and often overstated field, and with that comes confusion, inflated expectations and the risk of treating psychedelics as a solution in themselves.
In my recent conversation with psychiatrist Dr William Van Derveer on The MindHealth360 Show, we explored a far more grounded and clinically useful perspective. Rather than positioning psychedelics as a miracle cure, Dr Van Derveer places them within a broader healing model that includes trauma, attachment, inflammation, gut health, lifestyle, spirituality and the deeper biological drivers of mental ill health.
It is an approach that feels especially relevant now. As interest in psychedelic treatment accelerates, what is needed is not more hype, but more nuance. Not a search for the next silver bullet, but a deeper understanding of how mental health recovery actually works.
Moving beyond the limits of conventional psychiatry
One of the most interesting aspects of Dr Van Derveer’s work is the path that led him beyond conventional psychiatry. In our conversation, he described how the limits of medication and talk therapy pushed him to look more closely at the broader terrain of mental illness and recovery.
This is a tension that many clinicians and patients will recognise. Conventional approaches can be essential and at times lifesaving, but they are not always enough for people whose mental health symptoms are being driven by multiple overlapping factors. When trauma, inflammation, gut dysfunction, nervous system dysregulation, immune imbalance and chronic stress are all part of the picture, symptom suppression alone may leave the deeper causes untouched.
What emerged from our conversation was a much wider map of care: one that looks not only at thoughts, emotions and diagnoses, but also at biochemistry, physiology, attachment, lifestyle and meaning. The whole person lens integrative mental health calls for.
Why functional medicine and psychedelic therapy may need each other
A central theme in my discussion with Dr Van Derveer was that functional medicine and psychedelic therapy are often best understood as complementary.
Functional medicine helps identify and address the biological terrain that may be shaping mental health: inflammation, nutritional deficiencies, microbiome disruption, immune dysregulation, toxic load and poor stress resilience. Psychedelic therapy, by contrast, may help people access deep emotional material, trauma, insight, self-compassion and spiritual experience in ways that are not always possible through ordinary therapeutic processes alone.
For many people, these dimensions are deeply intertwined.
A person may have profound psychological insight during psychedelic therapy, but still struggle to sustain change if they return to a body that is inflamed, exhausted, dysregulated or depleted. Equally, someone may improve their physiology significantly, but remain stuck in deeply patterned trauma responses, relational wounds or destructive beliefs. What Dr Van Derveer describes is a model in which both biology and biography matter.
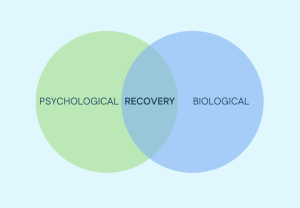
That is one of the strongest ideas from our conversation: recovery is often not either biological or psychological, but both.
Trauma is not only psychological, but physiological
Trauma is often misunderstood as something that exists only in conscious memory. In reality, as Dr Van Derveer explains, it may be stored outside narrative awareness, including in somatic, episodic and procedural memory.
This has important implications. Many people cannot easily explain why they feel the way they do, yet their nervous system, beliefs and behaviours may still be shaped by earlier experiences. Early attachment patterns and chronic dysregulation can influence not only relationships and emotional responses, but also inflammation, health behaviours and vulnerability to illness over time.
Psychedelic therapy may help people access this deeper material, but it does not replace the need for careful therapeutic support. Without integration and context, there is a risk of reducing complex healing processes to a single intervention.
Psychedelics are not a cure, but a catalyst
Public conversations about psychedelics often overlook an important distinction: these treatments are not cures in themselves.
As Dr Van Derveer emphasised, their value lies in their potential to act as catalysts. They may open access to insight, emotional processing and self-compassion. They may create opportunities for behaviour change and new perspectives. But they do not remove the need for ongoing therapeutic work, physiological support and meaningful changes in how a person lives.
Different compounds also play different roles. MDMA, ketamine and psilocybin each have distinct biochemical and psychological effects, and are suited to different contexts. A more mature understanding of psychedelic therapy requires this level of nuance, rather than treating all compounds or experiences as interchangeable.
Ultimately, the effectiveness of these treatments depends on what surrounds them. Insight alone is rarely sufficient. Lasting change tends to emerge when psychological work, biological support and lifestyle shifts are brought together.
A broader model of mental health care
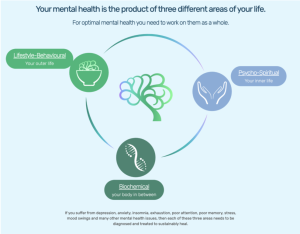
What becomes clear from this conversation is that the future of mental health care will depend on more integrated ways of thinking. Approaches that do not separate trauma from physiology, or biology from lived experience, but recognise how these layers interact.
Dr Van Derveer’s perspective reflects a growing shift towards understanding mental ill health as the result of multiple, interacting drivers. Addressing those drivers requires more than a single modality. It requires a framework that is capable of holding complexity while still offering practical pathways to healing.
This is where psychedelic therapy may have a role, not as a standalone solution, but as part of a wider system of care that addresses root causes and supports long-term change.
Listen to my conversation with Dr William Van Derveer on The MindHealth360 Show to explore how these approaches may work together in practice.
Thank you for reading.
Warmest wishes,
Kirkland Newman, Founder, MindHealth360
🌱 Your guide to root-cause mental health.
- The MindHealth360 Show – Subscribe for evidence-based conversations with leading clinicians and researchers, delivered to your inbox 🎧
- Integrative Medicine for Mental Health (IMMH) 2026 Conference – 4 days, 50+ speakers, up to 40 CE credits, exploring integrative medicine psychiatry and root-cause approaches to mental health ✉️
- Join the community – Ongoing insights, events and conversations shaping the field. Plus, free content when you sign up to the newsletter.